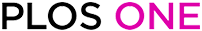Proposed hypothetical mechanism of keloid recurrence.
A. H&E showing cross section of Keloid lesion including adjacent normal skin. IL: intra-lesional; PL: peri-leisonal compartments; Pap. Dermis: papillary dermis; Ret. Dermis: Reticular dermis. B. Keloid fibroblasts may be changed, for example by mechanical injury itself or as a consequence of the healing process eg inflammation, and exhibit epigenetic differences to normal fibroblasts that allow paracrine signalling to occur. This may result in upregulated fibrotic markers that influence increased collagen and fibronectin deposition in a self-sustaining manner. C. At the margins of the lesion, keloid fibroblasts influence (paracrine signaling) normal skin primary fibroblasts to upregulate fibrotic markers such as CTGF, PAI-1, α-SMA. CTGF is known mitogenic for fibroblasts and PAI-1 is known to increase collagen deposition through inhibiting PA activity. CTGF may increase both collagen and fibronectin concomitantly. PAI-1 may also influence cell migration by stimulating PA receptor and β3 integrin cycling by endocytosis. α-SMA may also influence cell tension and adhesion. Collectively these changes may influence migration into the surrounding healthy skin leading to high recurrence of keloid lesion, post-surgery.